Translate this page into:
Amyloidosis and its clinical counterparts: still mysterious
-
Received: ,
Accepted: ,
How to cite this article: Garg M. Amyloidosis and its clinical counterparts: still mysterious. J Hematol Allied Sci 2021;1(1):43.
A 54-year-old hypertensive lady came to OPD with complaints of fatigue. She also presented with multiple small, waxy, nodular, non-itchy, non-progressive bilateral periorbital wart-like lesions [Figure 1] and a few similar lesions on fingers since last 2 years. On examination she had moderate pallor with no palpable organomegaly. Complete hemogram showed normocytic hypochromic anemia (Hb - 9.2 g/dl) and initial anemia workup did not reveal any significant abnormality. Further investigations revealed raised ESR (88 mm/hour) with normal other biochemical parameters. Thinking a provisional diagnosis of xanthelasma, lipid profile was done which was normal. Finally, skin biopsy was done which showed thick bundles of collagen throughout dermis with few showing pink staining amorphous material and pink staining deposits within blood vessels wall suggestive of amyloidosis. Further workup showed M band (0.71 g/dl) on SPEP, IgG kappa on IFE, SFLC ratio being 105.4 with 24 hours urine protein being 4174 mg/24 hour. Bone marrow aspirate showed 13% clonal plasma cells with kappa restriction and normal cytogenetics. Echocardiography showed normal ejection fraction with mild concentric left ventricular wall hypertrophy. This case highlights that amyloidosis can be deceiving and can present like benign-looking xanthelasma with complaints of only fatigue unlike deranged renal, cardiac function and typical Racoon’s eye, macroglossia, organomegaly typically seen in this disease.
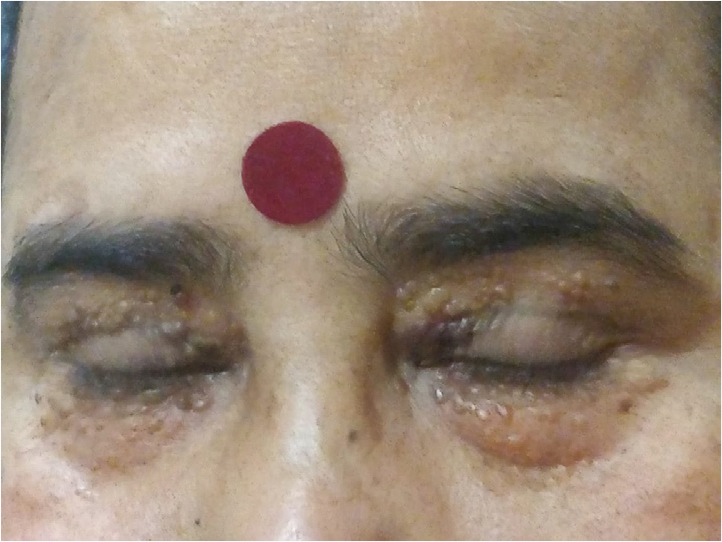
- Image showing bilateral, multiple, waxy, periorbital lesions.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.





